You are here: Home > Our Services > Specialised Procedures > Gastro-oesophageal Reflux Disease – Laparoscopic treatment of Hiatus Hernia
Gastro-oesophageal Reflux Disease – Laparoscopic treatment of Hiatus Hernia:
Nissen Fundoplication & LINX® Reflux Management System.

Mr Dhiren Nehra MPhil, FRCS
Consultant Surgeon, St Anthony's Hospital
For appointments 0208 337 6691, 01372 221 441, 0208 335 4501
Email:
website: www.mrdnehrafrcs.com
What is a Hiatus Hernia
It is an anatomical abnormality in which part of the stomach protrudes through the diaphragm and up into the chest.
Reflux disease is often associated with presence of a hiatus hernia. Typical symptoms of this condition are heartburn and regurgitation. Nearly 40% of the population in the Western countries will suffer from these symptoms at least once a month with 15% experiencing significant symptoms to seek medication in the form of acid suppression therapy. Long term exposure of the lower gullet to acid may cause a change in the lining namely Barrett’s oesophagus. This condition is precancerous and requires to be monitored.
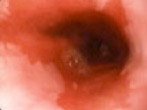
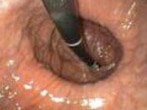
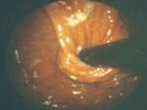
Endoscopic view of a) Barrett’s Oesophagus b) Hiatal hernia and c) following surgical repair with fundoplication
Apart from acid some patients complain of a bitter or bile taste in the mouth. Bile reflux has been a subject of my research and I have written widely on this subject. Whilst there is very effective treatment for acid reflux with drugs such as PPI omeprazole (Losec) and lanzoprazole (Zoton), some patients are intolerant to medication or their symptoms are so severe as to interfere with their day to day activity and affect sleep or some suffer from persistent cough and chest infections due to reflux. In such patients I offer to perform a keyhole surgical treatment called a Laparoscopic Nissen fundoplication. In this procedure the hiatus hernia is repaired and the stomach wall is used to create a wrap around the lower end of the gullet to 'strengthen' its weak muscle sphincter.
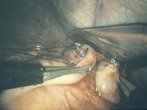
Kehole surgery for Reflux disease – Laparoscopic Nissen Fundoplication
Augmentation of the lower oesophageal sphincter using bead technology (LINX® Reflux management system)
The LINX® System is a novel technology, designed to magnetically augment a defective lower oesophageal sphincter, restore the barrier to reflux, and eliminate the symptoms and consequences of gastro-oesophageal reflux disease.
The magnetic sphincter augmentation device consists of a series of titanium beads, each with a magnetic core. These beads are linked together with independent titanium wires to form a flexible band that is placed around the distal oesophagus. The magnetic attraction between the beads provides a sustained force to augment the lower oesophageal sphincter, keeping it in the naturally closed position. During swallowing however, the device expands, with exponential reduction of the magnetic force between the beads as distension increases.
The device is implanted using keyhole surgery, and performing the procedure is substantially less complex and time-consuming than a laparoscopic nissen fundoplication. It does not alter the anatomy in the way that a fundoplication does, resulting in less side effects (it is also potentially removable and hence reversible).
The LINX® System is therefore an encouraging new technology for effective and permanent GORD treatment, eliminating either the requirement for long-term drug therapy or complex surgery.
How to relieve heartburn
- a) Lifestyle measures – reduce weight, cease smoking, avoid spicy and fatty food, wear loose clothes, elevate head end of bed or use 2-3 pillows when asleep.
- b) Medication - Simple antacid such Gaviscon for the occasional mild symptoms. Proton Pump inhibitors such as omeprazole and lansoprazole for established disease.
- c) Surgery – Laparoscopic Nissen Fundoplication. Magnetic Bead Technology.
I would advise anyone to seek medical consultation if symptoms are severe or persistent despite medication or if you have difficulty in swallowing. You may undergo OGD which involves examination of the gullet, stomach and duodenum with an endoscope. Specialised tests include oesophageal manometry and 24hr pH monitoring are used to assess extent of reflux and function of the gullet.
Information provided by Mr Dhiren Nehra MPhil. FRCS